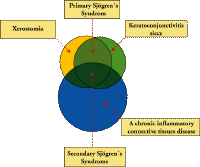
| Sjögren's syndrome |
|
| The salivary glands. This clinical entity - Sjögren's syndrome - which includes kerato-conjunctivitis sicca, xerostomia, probably depends on the presence of activated T-lymphocytes and hyper reactive B-lymphocytes in exocrine organs. The auto immune behavior of these lymphocytes expresses itself by producing a large number of non-specific antibodies, which can be demonstrated by laboratory investigation. The parenchyma of all the salivary glands reveals destruction of the ductules, creating rnvoepithelial islands. The acini are gradually lost. There is swelling of the major glands, at times with redness and pain. In cases of purulent flow, Streptococcus viridans, Klebsiella, or Enterobacteriaccae can be cultured. While the 'primary' Sjögren type is seen in all the salivary glands, a gland biopsy, from the lower lip confirms the diagnosis if accumulation of IgM and IgG is demonstrated. Characteristic in sialography is the irregular globular ectasy. Ductectasy is uncommon in early stages and suggestive for ascending bacterial inflammation secondary to the loss of continuing salivary flow. In sialochemistry the most striking lesion is the elevated permeability of the ductal lining to compare only with findings in mumps and acute allergic reactions. It is responsible for very high sodium levels and decreasing potassium concentrations in saliva samples. The final stage shows invariable the loss of protein synthesis. Apart from the high ESR, elevated gamma globulin and the appearance of SS-A (Ro) and SS-B (La) in blood chemistry indicating the actual situation the salivary amylase in serum (total amylase minus pancreas amylase) is a reliable parameter for the loss of functional glandular tissue. |